- What is Urolithiasis?
- What types of urinary stones are there?
- What are the Risk Factors of Urolithiasis?
- What are the signs and symptoms in Urolithiasis?
- How is Urolithiasis diagnosed?
- How is Urolithiasis treated?
- How are stones removed?
- How should the patient be followed up?
- How can Urolithiasis be prevented?
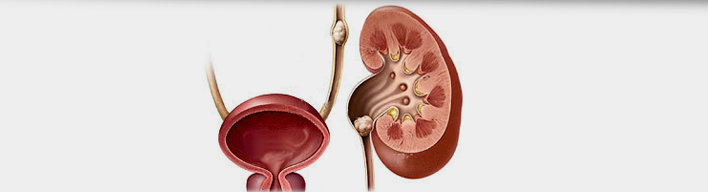
What is Urolithiasis?
Urolithiasis -or else called Urinary Calculosis- is the formation of stones (calculi) anywhere in the urinary tract (in the renal pyelocalyceal system, ureter, bladder, urethra). It is the third most common urinary tract disease in humans, following urinary tract infections and prostatic diseases. According to localization, there is renal lithiasis (nephrolithiasis), ureter lithiasis (stones in the tubules through which urine flows from kidneys to the bladder), bladder lithiasis and urethral lithiasis (stones in the tubule ejecting urine from the bladder outwards).
What types of urinary stones are there?
Urinary stones are classified according to their chemical composition.
- Calcium-based stones. This is the most common type of stone occurring more frequently in men aged 20-30 years old. Calcium binds with other substances, such as oxalates and phosphorus, and finally the stone is formed.
- Cystine Stones. They occur in patients suffering from Cystinuria, a hereditary disease afflicting both genders.
- Struvite stones. They are usually formed in women suffering from urinary tract infections. These stones may become very large in size.
- Uric acid stones. They occur more frequently in men than women. Patients undergoing chemotherapy are a high risk group for developing uric acid stones.
- More rare types of stones are formed in patients taking drugs, such as Aciclovir, Indinavir and Triamterene.
What are the risk factors of Urolithiasis?
Urinary stones are related with various risk factors that have to do either with each person's temperament (endogenous risk factors) or with the environment (exogenous risk factors). Usually there is a combination of both endogenous and exogenous factors leading to the formation of stones.
Endogenous risk factors include:
- Age - Stones are more common at the age group 20-50 years old.
- Gender - Urolithiasis occurs 3 times more frequently in men than in women.
- Family history/ Heredity - About 25% of patients with urolithiasis report that there is or was another member of their family with the same problem.
Exogenous risk factors inclue:
- Climate conditions: People living in warm climates are more likely to develop stones.
- Nutrition: High consumption of salt, animal albumen and fat is strongly associated with stone formation. Also, as opposed to what is widely believed, high calcium consumption (dairy products) also favors the development of stones.
- Obesity: High body weight predisposes stone formation.
- Fluid intake: Low fluid consumption -particularly if it is less than 1,5lt/day- increases the risk for the development of stones. Even water hardness is a factor related to high stone rate.
- Vocation (job): People with a more mental and sedentary vocation have higher risk for developing stones compared to those having a manual or more physical vocation.
- Pharmacotherapy: Specific antihypertensives, antiacid agents and therapies for immunosuppresed patients (e.g. HIV patients) predispose the formation of stones.
What are the signs and symptoms in Urolithiasis?
Many patients with urinary stones have no signs at all. The first symptoms occur when some stone moves to the ureter inhibiting urine flow from kidneys. The most common symptom is renal colic, that is strong pain in the region of kidneys, bladder or external genitalia. Pain usually occurs abruptly, is not relieved when changing position and is usually accompanied with nausea or even vomiting. There is often hematuria, which is microscopic -discovered in the general urine test- and, more rarely, macroscopic -visible in the urine. Sometimes, when there is concomitant urinary tract infection, urolithiasis may present symptoms such as shivering, fatigue, dysuria (painful micturition) and renal pain. Many are the times that urolithiasis is diagnosed accidentally when the patient undergoes imaging screening for some other irrelevant reason.
How is Urolithiasis diagnosed?
The diagnosis is based on the patient's history, clinical examination and on required laboratory and imaging screening tests. The history and clinical examination set the suspicion for lithiasis to the Urologist and diagnostic tests aim at confirming the diagnosis, investigating functionality and morphology of the urinary tract and identifying potential etiological factors that may be involved in stone formation. Screening tests required for the investigation of urolithiasis are divided in imaging and laboratory tests. The therapist physician will recommend which tests are necessary according to the case.
Imaging screening tests:
- Plain X-ray of kidneys, ureters and bladder (KUB X-ray): It traces about 80-90% of stones. However, there are stones (such as uric acid stones) that are not visible with KUB X-ray.
- UltraSound (U/S) of the urinary tract:: It provides information on the presence of obstruction (hydronephrosis) and can trace stones located in the kidney or bladder, but not in the ureter.
- Intravenous Urography or Pyelography: It demonstrates the exact location of stones, as well as any anatomic abnormalities that may exist and predispose stone formation. It is also useful for evaluating renal functionality and the degree of hydronephrosis.
- CTscan without contrast medium: Today this is the screening method of choice used in most urological centers for investigating urolithiasis, as it is diagnostically superior to intravenous urography and provides high-resolution imaging of renal anatomy.
Laboratory tests:
- General urine test (Urinalysis): There are usually red blood cells (erythrocytes) in the urine and sometimes there are also elements of urinary tract infection.
- Biochemical blood analysis: Measurement of urea, creatinine, uric acid and calcium in serum plasma.
- Parathormone: Hormone secreted by the parathyroid glands; it is measured in cases of high calcium values, for there may be glandular overfunction that contributes to stone formation.
- 24-hour urine collection: The aim is to determine the patient's metabolic condition for identifying any potential metabolic abnormality that could be responsible for stone formation.
- Stone analysis: Once the stone is removed, it is analyzed in specialized laboratories to identify the type of stone and take the proper measures that are necessary for reducing the chances of urolithiasis recurrence and relapse.
How is Urolithiasis treated?
Treating symptoms
During the phase of strong pain (renal colic), special pharmaceutical agents are administered to relieve the patient from pain. These agents come in injectable form called 'Non-steroid Anti-inflammatory Drugs' (NSADs) acting as pain relievers and reducing local edema. If pain persists, stronger analgesics can be administered, such as opioid analgesics. For preventing further renal colic attacks, oral NSADs are administered for 7 days; an inhibitor of a-adrenergic receptors can also be administered (usually given to men for prostate hyperplasia).
Immediate intervention is required only in a small number of patients, when:
- pain persists despite pharmaceutical treatment
- obstruction impairs renal function
- there is also urinary tract infection with fever
In these cases, there may be need for a pig-tail catheter to be placed. With the use of special instruments inserted through the urethra, the physician reaches the bladder and advances the catheter through the ureter to the kidney. In case this is not feasible, the tubule is inserted through the skin (percutaneous nephrostomy). If possible, the stone is removed at the same time.
Pharmacotherapy
With some types of stones, the therapist physician may prescribe medication aiming at either reducing the size of stone or preventing its reformation. Pharmacotherapy depends on the stone composition and presence or absence of metabolic disease.
How are stones removed?
Stone removal depends on the size and location of stone in the urinary tract. When the stone is less than 1cm in size and treated pharmaceutically, in 70% of cases the stone will automatically subside on its own within a period of 4-6 weeks. In the rest of the cases, there will be need for invasive therapy aiming at the fragmentation and removal of the stone/s.
Invasive methods include:
- Extracorporeal Shock Wave Lithotripsy (ESWL): The stone is broken with the use of shock waves. It is usually well tolerated by the patient and has 90% success rate. However, there are still some stones which cannot break with ESWL.
- Ureteroscopy and Intracorporeal Lithotripsy: It is used for removing stones located in the ureter. The ureteroscope is inserted through the urethra into the ureter until localizing the stone and removing its fragments. The most modern method is Laser LIthotripsy.
- Percutaneous Nephrolithotripsy (PNL) : It is applied for removing large or/and dense kidney stones that do not break with extracorporeal lithotripsy. The nephroscope is inserted through the skin into the kidney, localizes the stone and breaks it up with the use of special ultrasonic or ballistic devices.
- Open Surgery: Today it is used only for very few selected cases.
How should the patient be followed up?
There is 10% recurrence rate after the first urolithiasis episode, while the rate increases to 30-40% within the next 5 years and to 50-60% within a decade. That is why follow-up should be individualized according to each one's predisposition. This follow-up will be determined by the therapist physician with renal-bladder ultrasound and plain x-rays of kidneys, ureters and bladder (KUB X-ray).
It is also imperative to take measures for avoiding urolithiasis relapse. Thus, patients should consume plenty of fluids (2,5-3 liters/day), have a balanced nutrition with vegetable fibres, avoid consuming large amounts of salt, animal albumen and fat and consume a moderate amount of dairy products. In addition, in the case of obese patients, loss of body weight and moderate physical exercise contribute significantly to reducing relapse risk. Such precaution measures may prevent stone recurrence in 75% of cases.
How can Urolithiasis be prevented?
Guidelines on Prevention of Urolithiasis, along with prevention of all urological diseases, are available in Uro/Prevent.