Scientific Editor: Editorial Board ISUD website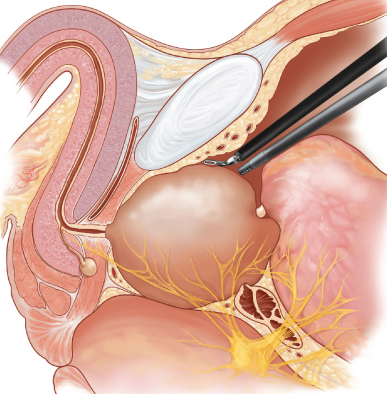
- What is Radical Prostatectomy?
- When is Radical Prostatectomy performed?
- What sort of preparation is required?
- How is the procedure performed?
- What about after Radical Prostatectomy?
- What is the effect on patient’s quality of life?
What is Radical Prostatectomy?
Radical Prostatectomy is the surgical procedure removing the entire prostate gland, along with the attached seminal vesicles and regional lymph nodes. It can be conducted as open surgery, laparoscopic or robotic.
When is Radical Prostatectomy performed?
Radical Prostatectomy is indicated when examinations reveal localized prostate cancer.
What sort of preparation is required?
Standardized preoperative preparation is carried out in hospital.
In case you are on anticoagulant therapy, suffer from severe heart/ lung health problems or have active urinary tract infection, you should always consult your physician.
How is the procedure performed?
Radical Prostatectomy can be open surgery (with skin incision), laparoscopic or robotic, and is performed under general anesthesia. In open surgery, the procedure can be also conducted after applying intrathecal anaesthesia, with the patient being awake feeling no pain though below the waist. There is usually need for placing a urocatheter. When open surgery is performed, a skin incision is made below the umbilicus, so that the surgeon can have access to the prostate. In the laparoscopic method, small skin incisions are made to allow for a small high-resolution camera to be inserted and transmit the image to the screen, as well as for multiple surgical instruments to pass through and be used by the surgeon and surgical group (usually 2 assistants). As for robotic-assisted surgery, this is based on laparoscopic surgery, with the only difference that all surgical instruments are connected to an apparatus giving the potential to the surgeon to operate while sitting in front of a screen using all instruments remote from the patient.
In Radical Prostatectomy, the surgeon removes the entire prostate gland, along with the attached seminal vesicles and regional lymphnodes.
In the end of the procedure, the bladder is reconnected to the urethra to restore urinary function. A catheter is placed postoperatively, which will be removed between the 7th and 15th postoperative day, depending on the case.
The length of hospital stay depends on the surgical method applied and the patient’s health condition. In most cases, hospital stay is 5-7 days for open surgery and 3 days for endoscopic surgery.
What about after Radical Prostatectomy?
Upon discharge from hospital, you will be given specific instructions about:
- when it is safe to restart your anticoagulant therapy
- when you can resume to intense physical activity and work
- what sort of antibiotic regimen you should receive postoperatively
What is the effect on patient’s quality of life?
You should be drinking plenty of fluids, so that urine is clear. It usually takes 14 days for the surgical wound to heal, and you may need up to 6 weeks to fully recover from surgery.
Erectile function may be lost in about 50-80% of patients who are operated, irrespective of the surgeon’s effort to preserve erectile nerves during surgery. In all patients (100%) there will be no longer postoperative ability to ejaculate or father a child by natural means.
Approximately 30% of patients may postoperatively have some degree of involuntary urine loss (incontinence), which in a small percentage may be severe and require permanent use of incontinence diapers or a second surgery to restore.
Lastly, it is essential to obtain histological results, for there may be need to receive some adjuvant therapy for cancer (e.g. radiotherapy or hormonal therapy). You should also have regular PSA check-ups throughout life, for if PSA values increase, you may need adjuvant cancer therapy (radiotherapy, hormonal therapy etc)


